OA Spiral Dynamic Unloading Knee Brace
$512.93Relieve your tibiofemoral and patellofemoral OA pain by choosing the BioSkin OA Spiral Knee Brace. It provides relief from both forms of OA pain and is easy to fit, apply and use.
Knee osteoarthritis is a result of deterioration of cartilage between the bones of the knee. When this happens, the bones start to come into contact with each other when you move your knee. As a result, this injury is known as a “wear and tear” type of disease. The main symptom of this condition is knee pain and inflammation, as well as tenderness and warmth of the knee. Some individuals will also develop bone spurs as a result of this condition. Some of the key risk factors leading to knee osteoarthritis are age, body weight and gender. To treat knee osteoarthritis, your doctor will usually aim to reduce your pain and discomfort as it is not possible to stop or reverse the cartilage deterioration. In severe cases, doctors may suggest various types of knee surgery of which knee replacement is usually the most aggressive option.
There are 3 knee bones that can play a role in the development of this condition – the femur (thighbone), patella (knee cap) and tibia (shinbone).
If your osteoarthritis is a result of deterioration of cartilage between the patella and the femur, you are suffering from patellofemoral osteoarthritis.
The cartilage between your femur and your tibia is in the form of two C shaped pieces and are known as menisci. If you are losing this cartilage between your tibia and femur, the diagnosis will be tibiofemoral osteoarthritis.
Another way of classifying the various types of knee osteoarthritis is into the primary and secondary categories:
In all cases, knee osteoarthritis usually comes on gradually and is not the result of a sudden traumatic injury like a fall or a blow to the knee.
Some of the key factors that increase the risk of developing knee osteoarthritis include the following:
Symptoms of this condition include the following:
In treating your knee osteoarthritis, your doctor will typically start with a conservative approach and then move to surgical intervention if the conservative approach is not successful.
It is important to appreciate that the cartilage deterioration that causes osteoarthritis cannot be stopped or reversed. As a result, the goal of conservative treatments will be to reduce the pain and discomfort you are suffering and to slow the rate of cartilage deterioration.
The conservative treatment approach can include the following:
If conservative treatments fail, your doctor may suggest surgical intervention to address your knee osteoarthritis. This can take one of the following forms:
Showing all 6 results

Relieve your tibiofemoral and patellofemoral OA pain by choosing the BioSkin OA Spiral Knee Brace. It provides relief from both forms of OA pain and is easy to fit, apply and use.
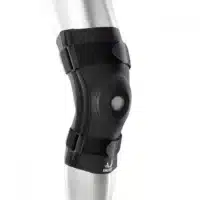
The Bio Skin Patella Stabilizer is an effective choice for treating patellar instability, anterior knee pain and other knee problems. Its donut shaped buttresses help to stabilize your patella and control swelling away while you remain comfortable and cool even during extended wearing periods.

The Bio Skin Patella Stabilizer with Conforma Hinge will help to treat anterior knee pain and other patellar instability related knee problems. Constructed from Bio Skin’s patented, breathable materials, the Stabilizer gives excellent compression to control swelling and decrease pain in the knee. The donut shaped buttresses stabilize the patella and help keep swelling away from the knee joint. The brace has a lightweight and comfortable hinge to help address problems of knee joint instability..

The Bio Skin Standard Knee Skin offers compression for pain relief, swelling control and greater proprioception. The two-panel construction design eliminates any seam from the sensitive skin behind the kneecap and the unique, patented Ultima material keeps it breathable and comfortable by wicking moisture away from the skin.

The Bio Skin Visco Knee Skin with Conforma Hinge is an excellent all-purpose knee support. The Visco gel ring around the patella provides passive massage to remove swelling and decrease knee pain. The brace is comfortable enough to wear all the time and is very useful a few weeks after knee surgery to control swelling and speed recovery. Includes Bio Skin’s innovative, lightweight and comfortable Conforma Hinge for extra knee joint stability.

The Bio Skin Visco Knee Skin with Thigh and Calf Straps uses a ring made from silicone that helps control swelling and relieve edema via passive massage.