BioLogix Knee Brace
$133.31The McDavid BioLogix Knee Brace combines a semi rigid lightweight design and bi-lateral aluminium dual axis geared hinges to provide a fluid feel and a natural range of motion.

Pain at the back of the knee, or posterior knee pain, can be a sign of any of five or six possible conditions, some of which are mild and easily treatable (or even ignorable). Others are potentially serious maladies requiring urgent medical attention.
In this article, we shall examine the 5 or 6 most common possible reasons for pain behind the knee and the treatments that doctors might adopt to resolve each possible cause.
One cause that we will not describe in detail for obvious reasons is a phenomenon described as “referred pain”. This is a situation in which you feel pain behind your knee but it actually originates somewhere else in your body, e.g. the front of the knee or even the lower back.
The accompanying symptoms of referred pain can span a wide range. With this type of pain, you will need to consult a doctor who can conduct tests to identify and treat the underlying cause.
One possible commonly experienced cause of pain behind the knee is a Baker’s cyst. This is a cyst that may be produced by an accumulation of synovial fluid in the “popliteal’ area behind the kneecap. Another name for this cyst is a “popliteal cyst”.
Synovial fluid actually occurs naturally in the knee (and other joints) and is required as a “lubricant” of the knee joint so that you can easily extend and flex the joint. A Baker’s cyst due to synovial fluid may cause some pain and discomfort. However, although these symptoms may vary over time and cause you some alarm, the condition is not inherently harmful. You can rest assured that you are not in danger of suffering long term damage to your knee.
In other cases, however, a Baker’s cyst may be an accumulation of inflammation behind the knee that is due to the effects of either arthritis or a knee injury such as a torn meniscus.
In either of the latter two cases, a Baker’s cyst will need to be addressed by treating its underlying cause, whether this is arthritis or a knee soft tissue injury.
In addition to treating its underlying causes, doctors may attempt to remove the cyst itself by one or more of the following methods:
Treatment of a Baker’s cyst that is due to an arthritic condition such as osteoarthritis or rheumatoid arthritis will likely continue for the rest of your life. These (and other) forms of arthritis do not have any fundamental cures that will halt or reverse the underlying knee damage. Instead, doctors will try to manage the condition by slowing its rate of progression and preserving as much of your quality of life as they can.
The pain at the back of your knee may also be due to an infection there.If an infection is present, the posterior knee pain would be accompanied by redness, warmth and possible swelling.
An infection could be one of three possible types:
Doctors can deploy a wide range of antibiotics to treat a possible infection. Your first step should be to contact one and schedule an appointment for medical advice, diagnosis and treatment.
Infections should be treated as matters for urgent medical attention. If they are not attended to in a timely fashion, various complications can develop up to and including sepsis, which is a life threatening medical condition.
Another possible cause of pain at the back of the knee is a soft tissue injury in that reqion. The most common knee injuries that might result in this type of pain would be a ligament strain, a muscle or tendon strain or a torn meniscus.
The most common types of ligament sprain that can result in posterior knee pain are tears or overstretching of the posterior cruciate ligament (pcl) (but not of the anterior cruciate ligament (acl)).
Where muscle or tendon strains are concerned, the injury most likely to cause posterior knee pain would be tearing or overstretching of the hamstring muscle (located at the back of the thigh).
Accompanying symptoms (in addition to pain behind the knee) would be one or more of the following:
A severe hamstring strain may be accompanied by occasional muscle spasms.
If you have experienced either a ligament sprain or meniscus tear, you may have difficulty walking without feeling knee instability, i.e. that the joint may give way beneath you.
The symptoms will likely be at their most severe during a period of activity, and will tend to recede during periods of rest.
In the main, doctors will treat these types of knee soft tissue injuries using the R.I.C.E. protocol:
In addition to these treatments, doctors will probably refer you to a therapist who can devise a physical therapy exercise program for your knee to help you return to activity as soon as possible and with as little risk of re-injury as possible.
We mentioned knee arthritis above as a possible cause of a Baker’s cyst behind the knee.
However, if the posterior knee pain and cyst are due to arthritis of the knee, that will need to be managed separately. There are several types of knee arthritis, and the more likely ones are:
Arthritis typically causes knee pain and stiffness that may be worse upon awakening in the morning or after a period of inactivity (e.g. a daytime nap).You may also suffer from swelling and inflammation because of the condition.
If you think your pain behind the knee is due to arthritis, you should see a doctor who can make a formal diagnosis and rule out the other potential causes mentioned in this article.
Once arthritis has been positively identified, doctors can recommend a range of drugs depending on the type of arthritis that you have.
They can also refer you to an occupational therapist who can advise on home modifications to reduce the pain of performing daily activities like cooking, bathing and toileting. A physical therapist can devise an exercise program that will help you maintain knee joint function and range of motion.
If you have knee osteoarthritis, you can try wearing an unloader knee brace that will slow the rate of progression of the disease.
As far as surgery is concerned, doctors once again have a range of options up to and including knee replacement.
For additional information on the treatment and management of knee arthritis, please read this article.
These (whether malignant or benign) are another potential cause of pain behind the knee. Clearly, this is a very serious problem and you should consult a doctor as soon as possible for a complete examination, diagnosis and treatment.
To say any more on this subject would be beyond the scope of this article.
This is a condition caused by the appearance of a blood clot in a deep vein, typically in one of your legs.Although deep vein thrombosis (DVT) can occur with pain behind the knee (typically the calf area) it is important to note that it can also occur with no symptoms at all.
DVT can be a serious and potentially life threatening condition, since the blood clot can break off and travel in your bloodstream to your lungs. There it can block blood flow and cause what is called a pulmonary embolism.
The symptoms that accompany the posterior knee pain may include swelling of the leg with the clot, red or discolored skin and a “warm to the touch” feeling in the leg. As mentioned though, in some cases, DVT can be present with no noticeable symptoms.
If you think that your pain at the back of your knee may be a result of Deep Vein Thrombosis, you should consult a doctor without delay for a proper diagnosis.
If your doctor confirms your suspicion, the goals will be to prevent the blot clot from expanding or breaking loose. Treatment will also be aimed at preventing the formation of another clot.
Your doctor can prescribe blood thinning medication to achieve these goals, such as Heparin, Warfarin or dabigatran. These won’t break up the clots you already have, but they will help to prevent them expanding or increasing in number.
If your clot presents an immediate risk, clot busting drugs can be injected directly via IV or even directly into the clot. As an alternative, a surgeon can inject a filter into a large abdominal vein to prevent the blood clot reaching your lungs even if it does break off.
To manage the risk of a blood clot developing, you can wear compression stockings. Choose stockings that apply graduated compression between your feet and your knees as that is the portion of your legs where DVT is most likely to develop.
Showing all 9 results
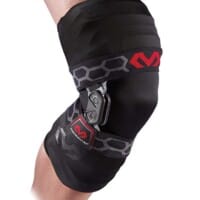
The McDavid BioLogix Knee Brace combines a semi rigid lightweight design and bi-lateral aluminium dual axis geared hinges to provide a fluid feel and a natural range of motion.

The Mueller Sports Medicine Green Adjustable Knee Brace offers optimal support for weak, injured and arthritic knees. One size. Fits either knee.
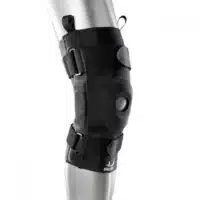
The Bio Skin Hinged Knee Skin uses offset, bi-centric aluminium hinges to conform to the contours of differing leg shapes and provide extra knee support.

The Bio Skin Hinged Knee Skin – Front Closure uses offset, bi-centric aluminium hinges to conform to the contours of differing leg shapes and provide extra knee support. In addition, it has a hook & loop front closure design to simplify application and removal and to help it accommodate a wide variety of leg shapes.

The McDavid Knee Brace With Dual Disk Hinges features an open centred 360˚ padded buttress to isolate and support your patella, as well as bound edges that help prevent irritation. In addition, a perforated back panel provides heat and moisture management and all-around comfort.

The Bio Skin Premium J with Conforma hinge combines function, comfort and affordability with a buttress around the patella to help prevent patella subluxation and knee dislocation. It also features dual elastic straps criss-crossing the knee to help seat the patella in its trochlear groove for less patellofemoral pain.

The DynaPro Reusable Cold & Hot Compress is a versatile non-toxic compress that you can use for both hot and cold therapies and for treatment of both acute and chronic injuries.

The DynaPro Health Single Use Instant Cold Pack is an essential part of a first aid kit that will help you start treatment of acute injuries right away.

Kego Walking Crutches (Pair) are durable lightweight crutches manufactured from aluminium. They will provide you with stability if you are unable to walk on your own. The crutches are equipped with a comfortable and durable underarm pad and hand grip. These walking crutches are sold in pairs. They are available in four crutch sizes –…